Is Insomnia Genetic? What Twin Studies and Epigenetics Actually Tell Us
If someone in your family has always been a terrible sleeper, you’ve probably wondered whether you inherited more than just their nose. It’s a fair question, and it has a real answer. Not a tidy one, but a genuinely interesting one.
The short version: genetics plays a meaningful role in insomnia, but “meaningful” is not the same as “decisive.” What the research actually shows is more nuanced than either “it’s all in your genes” or “just fix your sleep habits.” And the nuance, it turns out, is genuinely reassuring.
The Short Answer: Partly, Yes
Twin studies are the gold standard for unpicking genetic from environmental influences, and the insomnia research here is fairly consistent. Two independent meta-analyses published in 2021 converged on roughly the same estimate: genetic factors account for around 40% of the variance in insomnia, with a second meta-analysis of thirteen independent samples arriving at a nearly identical figure of 39%.
That 40% figure is worth sitting with. It tells us that genes matter. It also tells us that 60% of the picture is something else entirely, shaped by environment, behaviour, life experience, and the choices we make around sleep.

Heritability statistics describe how much of the variation between people in a population can be attributed to genetics. They don’t tell you anything definitive about any one person. Two people can carry the same genetic variants and have completely different sleep outcomes. Heritability is a population-level number, not a personal prophecy.
What Are We Actually Inheriting?
There isn’t a single “insomnia gene” sitting in your DNA waiting to ruin your nights. Insomnia is polygenic, meaning it involves contributions from many genetic variants, each with a small effect. What these variants appear to influence most is the reactivity of your nervous system, particularly how your sleep-wake system responds to stress.
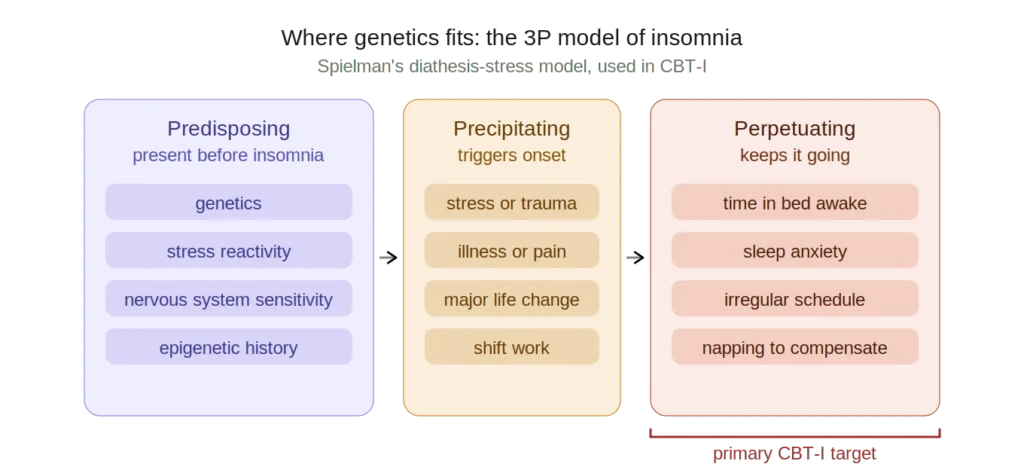
Sleep researchers have long conceptualised insomnia through what’s called the 3P model: predisposing factors, precipitating events, and perpetuating behaviours. Genetics sits squarely in the first category. What you may be inheriting isn’t insomnia itself, but a nervous system that is more reactive to disruption, more alert to threat, and slower to power down under stress. A 2023 systematic review in the Journal of Sleep Research described insomnia as a complex polygenic stress-related disorder likely caused by a synergy of genetic and environmental factors, with stress-related sleep reactivity being the key inherited trait.
In other words, the genetic piece may be less about sleep and more about stress.
Genes Aren’t a Static Script: The Role of Epigenetics
Here’s where it gets genuinely fascinating. Genetics isn’t as fixed as most people assume. Enter epigenetics: the study of how your environment, experiences, and behaviours influence which genes get expressed and to what degree, without changing the underlying DNA sequence itself.
Think of your genome as a piano. Epigenetics is about which keys get pressed and how often, not whether the keys exist. Two people can have the same piano and produce entirely different music depending on what they’ve been through.
Research reviewed by Palagini and colleagues suggests that insomnia may develop and be maintained through epigenetic stress-response mechanisms, where stressful life experiences leave chemical marks on genes involved in sleep regulation. These modifications don’t rewrite your DNA. But they can change how your brain responds to stress, with downstream effects on sleep. Chronic stress, early-life adversity, and ongoing sleep disruption itself all appear to influence gene expression in ways relevant to insomnia.

This is important because it means the line between predisposition and expression isn’t fixed. Having the predisposition doesn’t guarantee the expression. And even where genes have been expressed in ways that contribute to insomnia, that expression is not immutable.
Predisposition Is Not Destiny
This distinction matters more than people realise. A genetic predisposition to insomnia is a bit like a genetic predisposition to high blood pressure. It raises your risk. It means certain things, like sustained stress, irregular schedules, or learned patterns of anxious wakefulness, may hit harder for you than for someone without that predisposition. It doesn’t mean you’ll inevitably have a problem, and it certainly doesn’t mean the problem is untreatable if it develops.
The perpetuating factors that transform a bad patch of sleep into chronic insomnia are overwhelmingly behavioural and cognitive: lying in bed awake for long periods, extending time in bed to compensate for poor sleep, developing anxious associations with the bedroom, ruminating at night. These patterns are something a nervous system with higher stress reactivity may be more prone to developing. But they’re still learned patterns. And learned patterns can be changed.
Does Genetic Predisposition Affect Whether Treatment Works?
This is perhaps the most practically important question. The answer, based on available evidence, is no.
Research on CBT-I efficacy has found no significant relationship between genetic predisposition to insomnia (as measured by higher stress reactivity) and treatment outcomes. CBT-I works by targeting the perpetuating factors that keep insomnia going, regardless of what started it. A broader review of CBT-I effectiveness noted that outcomes are not moderated by age, sex, use of sleep medications, or comorbidity. Genetic predisposition isn’t on that list either.
What happens in a CBT-I treatment programme isn’t about reprogramming your nervous system’s baseline temperament. It’s about changing the conditioned responses, behaviours, and thought patterns that have accumulated around sleep. A more reactive nervous system may have made you more vulnerable to developing those patterns. But the patterns themselves respond to treatment.
The Takeaway
Your biology may have made you a lighter sleeper, more sensitive to stress, or quicker to lie awake when life gets difficult. That’s real, and it’s worth knowing. But it isn’t a closed door.
Genetics sets the conditions. Epigenetics reminds us those conditions shift with experience. And decades of clinical research on CBT-I treatment for insomnia tell us clearly that what perpetuates insomnia is not what you inherited, but what your mind and body learned to do in response to it. That part is squarely within reach.
If you’re ready to understand what’s actually driving your insomnia and start working on it, book a free 15-minute consultation. We can talk through what treatment looks like and whether it’s a good fit.


