Insomnia During Perimenopause and Menopause: Why It Happens and What Actually Helps
You used to be a decent sleeper. Not perfect, maybe, but functional. Now you’re awake at 3 a.m., sheets kicked off, mind churning through tomorrow’s to-do list while your body can’t decide if it’s overheating or just restless. You’ve tried the chamomile tea, the lavender pillow spray, the “no screens before bed” rule. And yet here you are, exhausted during the day and wide awake at night.
If this sounds familiar, you’re in very large company. Sleep difficulties affect 40 to 60% of women during the menopausal transition, making menopause insomnia one of the most common and least discussed symptoms of this stage of life. The good news: this isn’t something you simply have to endure. There are effective, evidence-based approaches that go well beyond sleep hygiene tips, and most women haven’t heard of them yet.
 How Common Is Menopause Insomnia?
How Common Is Menopause Insomnia?
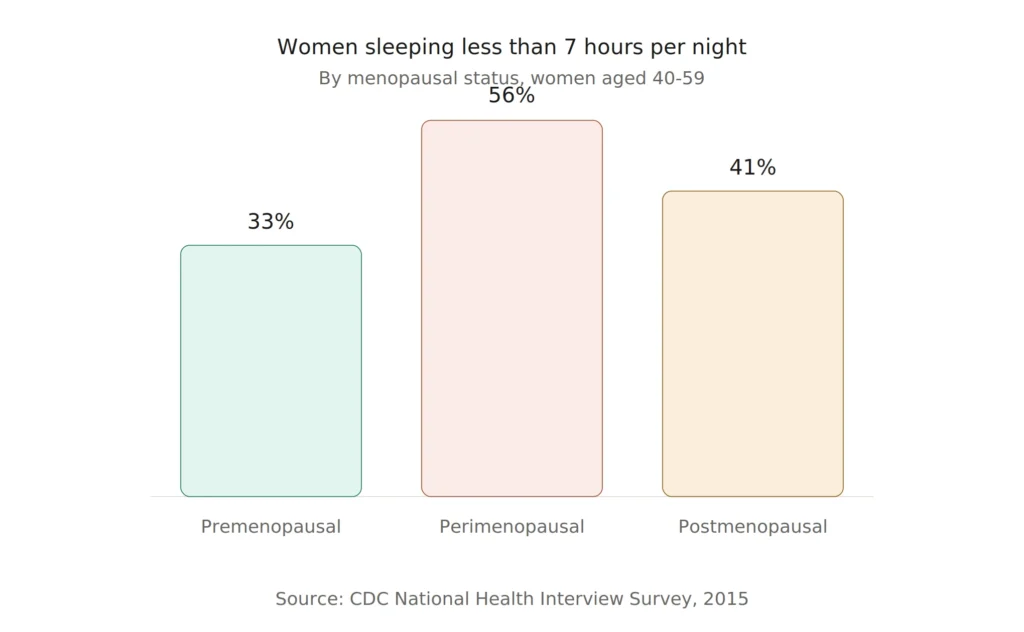
More common than most people realize. According to data from the U.S. National Health Interview Survey, 56% of perimenopausal women sleep less than seven hours per night, compared to 33% of premenopausal women. That’s a sharp jump, and it’s not subtle in how it feels.
The numbers hold up in longer-term research too. The Study of Women’s Health Across the Nation (SWAN), a 10-year longitudinal study of over 3,300 women, found that insomnia symptoms were present in 31 to 42% of perimenopausal women at any given annual check-in. Symptoms were more prevalent in late perimenopause than early, and up to 26% of women developed clinical insomnia severe enough to impair daytime functioning.
Canadian data tells a consistent story. The Canadian Longitudinal Study on Aging found that postmenopausal women were significantly more likely to meet criteria for sleep-onset insomnia disorder compared to pre- and perimenopausal women. And a separate analysis of Canadian health surveys found that women aged 40 to 59 showed a 29% increase in the likelihood of insomnia symptoms over a single decade, a trend the researchers linked partly to the menopausal transition.
These aren’t small numbers. And yet many women are told, implicitly or explicitly, that poor sleep is just part of the deal. It’s common, yes. But common doesn’t mean untreatable.
 Why Menopause Disrupts Sleep: The Hormonal Picture
Why Menopause Disrupts Sleep: The Hormonal Picture
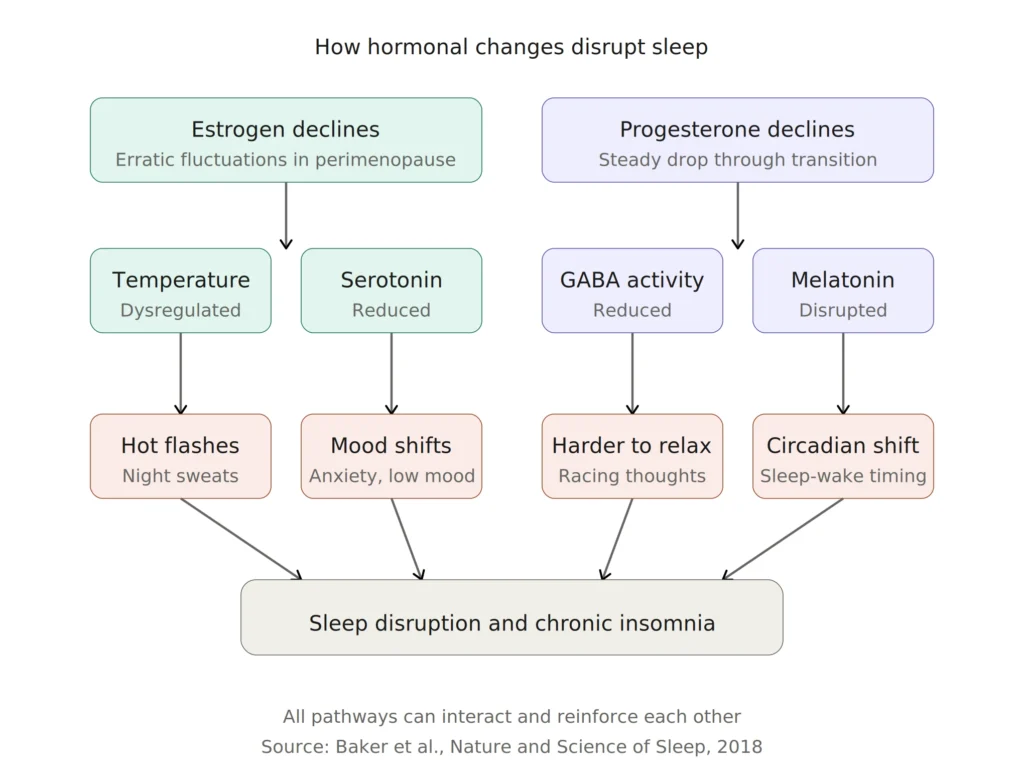
Estrogen, Progesterone, and Your Sleep Architecture
Your body’s sleep system doesn’t operate in isolation from your hormonal system. Estrogen plays a role in regulating body temperature, supporting serotonin production (which influences mood and sleep-wake cycles), and helping with melatonin production. Progesterone, sometimes called the “calming hormone,” boosts GABA activity in the brain, a neurotransmitter that promotes relaxation and makes it easier to fall and stay asleep. Together, these hormones help keep your sleep architecture intact: the cycling between light sleep, deep sleep, and REM sleep that allows you to wake up feeling restored.
During perimenopause, both estrogen and progesterone don’t simply decline in a straight line. They fluctuate erratically, sometimes surging, sometimes dropping. Research from the SWAN study found that increasing levels of follicle-stimulating hormone (FSH) were associated with greater sleep fragmentation, while decreasing estrogen was linked to difficulty falling and staying asleep. Notably, some researchers have found that it’s the degree of fluctuation in estrogen, not just the overall decline, that predicts sleep disruption. Your brain’s sleep-regulation systems are trying to hit a moving target.
Hot Flashes, Night Sweats, and the Chicken-or-Egg Question
Hot flashes and night sweats are often blamed as the primary culprits behind menopause insomnia. And they certainly don’t help. But the relationship is more interesting than it first appears.
Research from Johns Hopkins has shown that many women actually wake up just before a hot flash occurs, not because of it. Changes in the brain that trigger the hot flash also appear to trigger the awakening. This means the sleep disruption and the hot flash may share a common neurological origin rather than one simply causing the other.
That said, night sweats are genuinely disruptive. Waking up drenched and needing to change clothes or sheets fragments sleep in a very concrete way. And the more often you wake during the night, the more your sleep architecture breaks down. Studies have found that women with menopause-related insomnia spend significantly more time awake after initially falling asleep, with nearly half sleeping less than six hours per night.
 It’s Not Just Hormones: The “Menopause Puzzle”
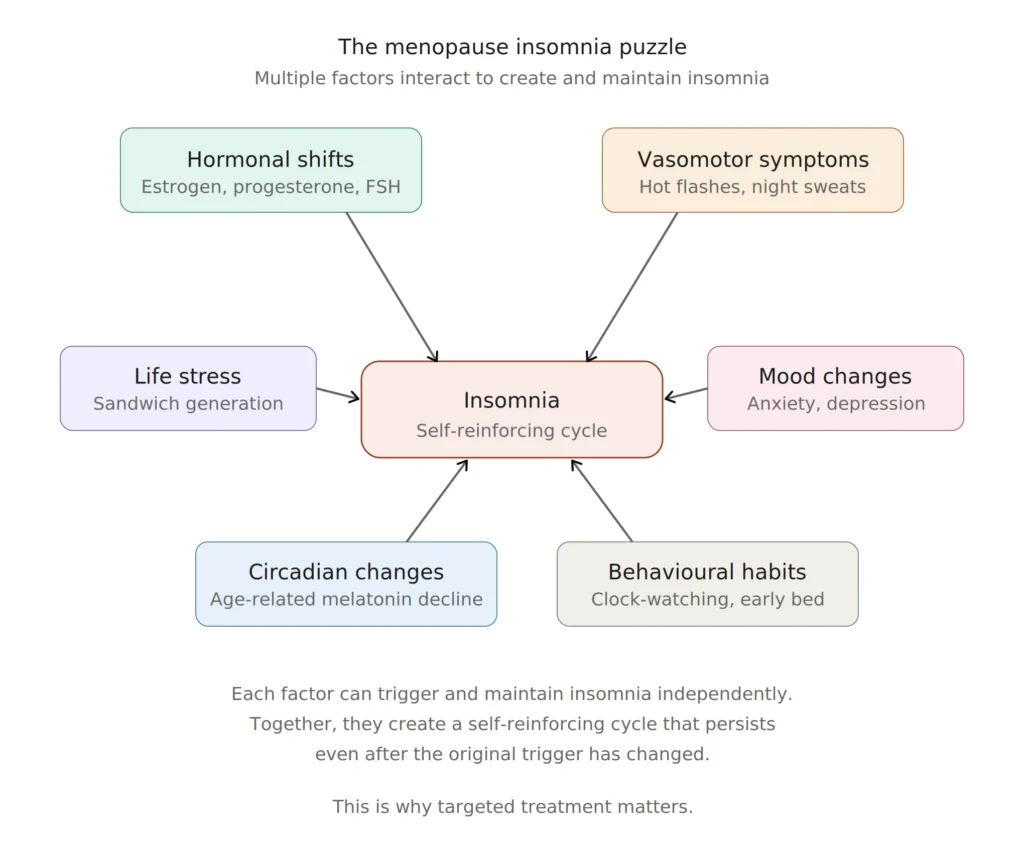
It’s Not Just Hormones: The “Menopause Puzzle”
If hormones were the whole story, the solution would be straightforward. But insomnia researchers sometimes call menopausal sleep disruption a “puzzle” because so many pieces interlock.
Many women going through perimenopause and menopause are also navigating what’s sometimes called the “Sandwich Generation” years: caring for aging parents while still supporting children, managing demanding careers, and processing significant life transitions. These stressors alone can fuel insomnia, and when they’re layered on top of hormonal shifts, the effect compounds. Understanding how chronic stress keeps the nervous system on high alert helps explain why so many women feel “tired but wired” at bedtime.
There’s also the circular connection between insomnia and mood. Anxiety and depression both increase during the menopausal transition, and both have a bidirectional relationship with sleep. Poor sleep worsens mood, and low mood makes sleep harder. Add in age-related changes to circadian rhythm and declining melatonin production, and you begin to see why no single factor explains the whole picture.
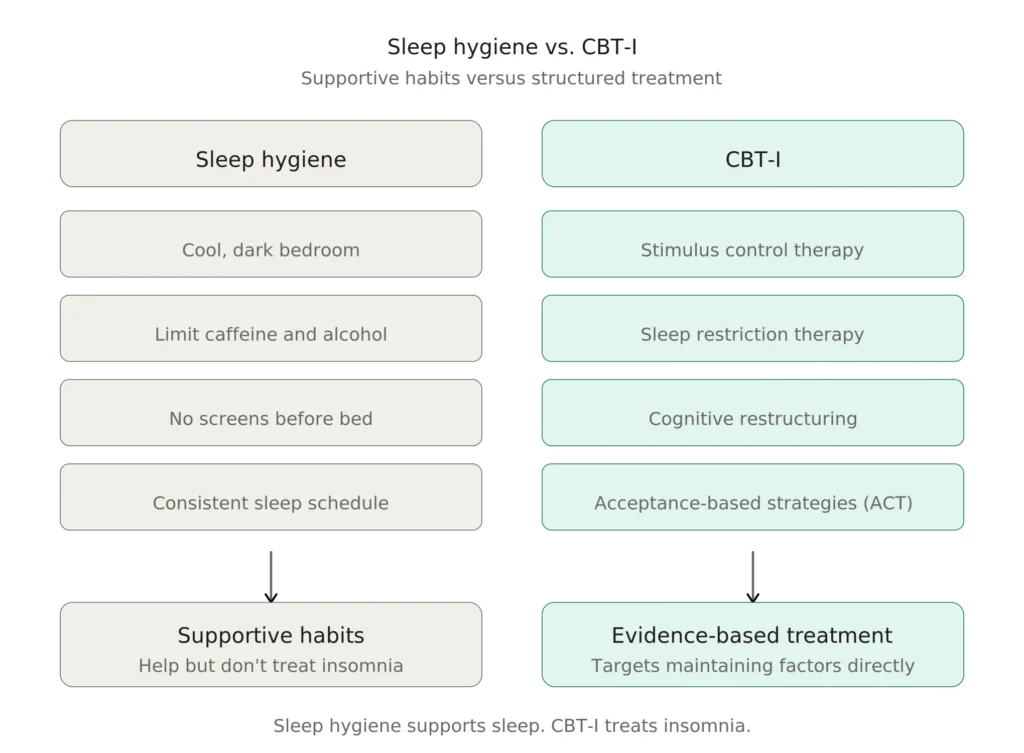
Why Sleep Tips Alone Don’t Fix Menopausal Insomnia
This is worth saying plainly: keeping your bedroom cool, avoiding caffeine after noon, and putting your phone away before bed are all reasonable habits. They support good sleep. But they are not treatments for chronic insomnia.
Sleep hygiene is a bit like flossing. It’s a good baseline practice, but if you have a cavity, flossing alone won’t fix it. When insomnia has become chronic, meaning it’s been disrupting your sleep at least three nights per week for three months or more, the problem has usually taken on a life of its own. Habits, thought patterns, and conditioned associations with your bed and bedroom start maintaining the insomnia independently of whatever originally triggered it.
 At that point, what’s needed is a structured intervention that directly addresses those maintaining factors. And that’s where most women hit a gap: they’re rarely told that such an intervention exists, is non-pharmacological, and has strong evidence behind it.
At that point, what’s needed is a structured intervention that directly addresses those maintaining factors. And that’s where most women hit a gap: they’re rarely told that such an intervention exists, is non-pharmacological, and has strong evidence behind it.
What Is CBT-I, and Does It Work for Menopause Insomnia?
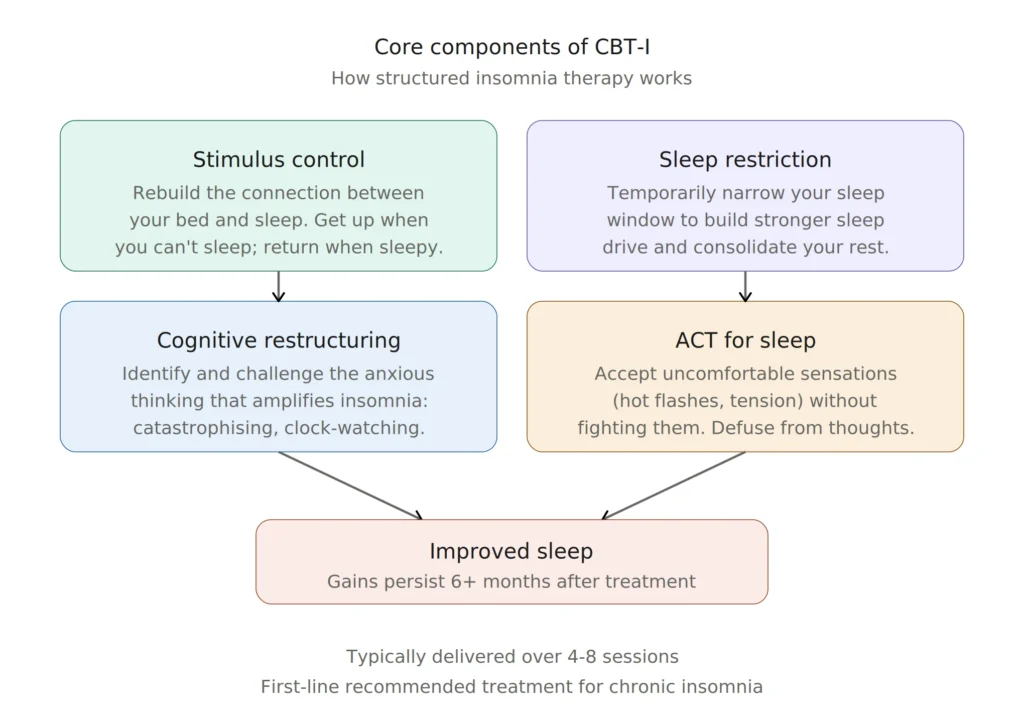
Cognitive Behavioural Therapy for Insomnia (CBT-I) is a structured, short-term therapy (typically four to eight sessions) that targets the behaviours, thought patterns, and conditioned responses that keep insomnia going. Its core components include stimulus control (rebuilding the association between your bed and sleep), sleep restriction (temporarily consolidating your sleep window to increase sleep drive), and cognitive restructuring (working with the anxious, frustrated thinking that tends to amplify sleep problems).
The evidence for CBT-I in menopausal insomnia is strong. A 2024 scoping review of randomized controlled trials found that CBT-I significantly improves sleep quality and reduces insomnia severity in menopausal women, with improvements persisting for up to six months after treatment ends. The MS-FLASH study, one of the largest trials to compare interventions for menopausal sleep problems, found that CBT-I was more effective than venlafaxine, escitalopram, yoga, aerobic exercise, omega-3 supplements, and estradiol for reducing insomnia symptoms.
That last point is worth sitting with. CBT-I outperformed medication, exercise, and even hormonal treatment for the specific problem of insomnia. It’s not that those other approaches don’t have value; they do, particularly HRT for vasomotor symptoms. But for the insomnia itself, CBT-I addresses the maintaining factors that other treatments don’t reach.
An important nuance: CBT-I doesn’t compete with HRT. They address different pieces of the menopause puzzle. HRT targets the hormonal drivers (hot flashes, night sweats, mood), while CBT-I targets the behavioural and cognitive patterns that have locked insomnia into place. For many women, the most effective approach involves both. Learning how CBT-I and ACT work together to treat chronic insomnia can also help with the racing thoughts and body-level tension that often accompany menopausal sleep difficulties. Acceptance and Commitment Therapy (ACT) techniques, like defusion from unhelpful thoughts and acceptance of uncomfortable body sensations, fit naturally alongside CBT-I for women dealing with hot flashes and nighttime anxiety.
 A client, a woman in her early 50s, came in convinced her insomnia was entirely about the hot flashes. And they were certainly part of it. But over the course of treatment, she began to see that the anxiety she’d built around sleep, the clock-watching, the early bedtimes to “catch up,” the growing dread as evening approached, were doing as much to maintain her insomnia as the night sweats were. Through CBT-I, she significantly reduced the number of times she woke during the night and found she could get back to sleep much more quickly when she did wake. More importantly, her daytime energy and mood improved. She described it as feeling like herself again.
A client, a woman in her early 50s, came in convinced her insomnia was entirely about the hot flashes. And they were certainly part of it. But over the course of treatment, she began to see that the anxiety she’d built around sleep, the clock-watching, the early bedtimes to “catch up,” the growing dread as evening approached, were doing as much to maintain her insomnia as the night sweats were. Through CBT-I, she significantly reduced the number of times she woke during the night and found she could get back to sleep much more quickly when she did wake. More importantly, her daytime energy and mood improved. She described it as feeling like herself again.
When Should You Seek Help for Menopausal Sleep Problems?
If your sleep has been consistently disrupted for three months or more, if you’re experiencing daytime fatigue, irritability, or difficulty concentrating, and if the frustration around sleep has started to feel like its own problem, those are good signals that it’s time to look beyond lifestyle adjustments.
It’s also worth knowing that the risk of sleep apnea increases after menopause, as the protective effects of estrogen and progesterone on the upper airway diminish. Sleep apnea in women can present differently than in men, sometimes looking more like insomnia, which means it can go undiagnosed. A conversation with your GP about screening is worthwhile, especially if you snore, wake with headaches, or feel excessively sleepy during the day despite spending enough time in bed.
If you’re curious about what structured insomnia treatment involves, you can read about what a first CBT-I session actually looks like. It’s less mysterious than you might expect, and knowing what to anticipate can make the step easier to take.
You Don’t Have to Wait This Out
Menopause insomnia is real, it’s common, and it has identifiable causes. But “common” and “inevitable” are not the same thing. The hormonal shifts are real. The hot flashes are real. The life stress is real. And the insomnia that grows out of all of it is also real, but it responds well to treatment that addresses how it’s being maintained, not just what started it.
If you’re in British Columbia and your sleep has been off the rails for longer than feels acceptable, you don’t need to keep white-knuckling your way through it. Book a free consultation and let’s talk about what’s going on with your sleep and whether CBT-I might be a good fit.


